The lymphatic system is a network of vessels and nodes which acts to drain lymphatic fluid from the tissues and return it to the circulation.
In this article, we shall look at the anatomy of the lymphatic drainage of the head and neck – the lymph vessels, nodes and their clinical relevance.
Lymphatic Vessels
The lymphatic vessels of the head and neck can be divided into two major groups; superficial vessels and deep vessels.
Superficial Vessels
The superficial vessels drain lymph from the scalp, face and neck into the superficial ring of lymph nodes at the junction of the neck and head.
Deep Vessels
The deep lymphatic vessels of the head and neck arise from the deep cervical lymph nodes. They converge to form the left and right jugular lymphatic trunks:
- Left jugular lymphatic trunk – combines with the thoracic duct at the root of the neck. This empties into the venous system via the left subclavian vein.
- Right jugular lymphatic trunk – forms the right lymphatic duct at the root of the neck. This empties into the venous system via the right subclavian vein.
Lymph Nodes
The lymph nodes of the head and neck can be divided into two groups; a superficial ring of lymph nodes, and a vertical group of deep lymph nodes.
Superficial Lymph Nodes
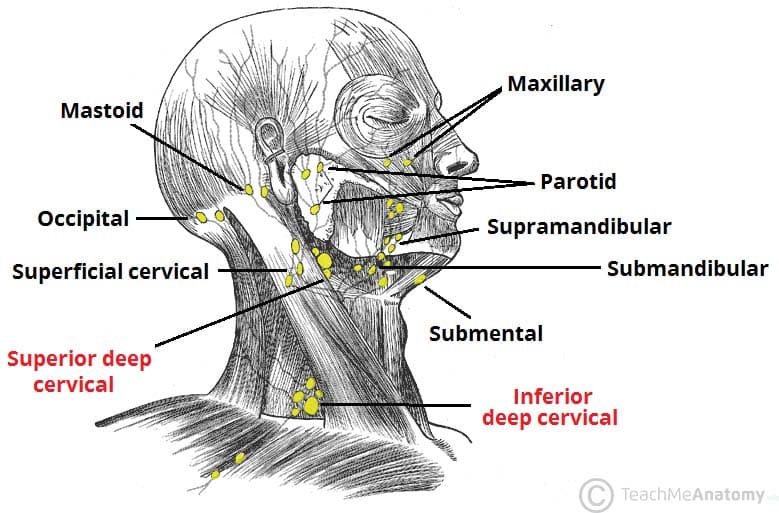
The superficial lymph nodes of the head and neck receive lymph from the scalp, face and neck. They are arranged in a ring shape; extending from underneath the chin, to the posterior aspect of the head. They ultimately drain into the deep lymph nodes.
- Occipital: There are usually between 1-3 occipital lymph nodes. They are located in the back of the head at the lateral border of the trapezius muscle and collect lymph from the occipital area of the scalp.
- Mastoid: There are usually 2 mastoid lymph nodes, which are also called the post-auricular lymph nodes. They are located posterior to the ear and lie on the insertion of the sternocleidomastoid muscle into the mastoid process. They collect lymph from the posterior neck, upper ear and the back of the external auditory meatus (the ear canal).
- Pre-auricular: There are usually between 1-3 pre-auricular lymph nodes. They are located anterior to the auricle of the ear, and collect lymph from the superficial areas of the face and temporal region.
- Parotid: The parotid lymph nodes are a small group of nodes located superficially to the parotid gland. They collect lymph from the nose, the nasal cavity, the external acoustic meatus, the tympanic cavity and the lateral borders of the orbit. There are also parotid lymph nodes deep to the parotid gland that drain the nasal cavities and the nasopharynx.
- Submental: These lymph nodes are located superficially to the mylohoid muscle. They collect lymph from the central lower lip, the floor of the mouth and the apex of the tongue.
- Submandibular: There are usually between 3-6 submandibular nodes. They are located below the mandible in the submandibular triangle and collect lymph from the cheeks, the lateral aspects of the nose, upper lip, lateral parts of the lower lip, gums and the anterior tongue. They also receive lymph from the submental and facial lymph nodes.
- Facial: This group comprises the maxillary/infraorbital, buccinator and supramandibular lymph nodes. They collect lymph from the mucous membranes of the nose and cheek, eyelids and conjunctiva.
- Superficial Cervical: The superficial cervical lymph nodes can be divided into the superficial anterior cervical nodes and the posterior lateral superficial cervical lymph nodes. The anterior nodes lie close to the anterior jugular vein and collect lymph from the superficial surfaces of the anterior neck. The posterior lateral nodes lie close to the external jugular vein and collect lymph from superficial surfaces of the neck.
Deep Lymph Nodes
The deep (cervical) lymph nodes receive all of the lymph from the head and neck – either directly or indirectly via the superficial lymph nodes. They are organised into a vertical chain, located within close proximity to the internal jugular vein within the carotid sheath. The efferent vessels from the deep cervical lymph nodes converge to form the jugular lymphatic trunks.
The nodes can be divided into superior and inferior deep cervical lymph nodes. They are numerous in number, but include the prelaryngeal, pretracheal, paratracheal, retropharyngeal, infrahyoid, jugulodigastric (tonsilar), jugulo-omohyoid and supraclavicular nodes.
Clinical Relevance: Virchow’s Node
Virchow’s node is a supraclavicular node, located in the left supraclavicular fossa (located immediately superior to the clavicle). It receives lymph drainage from the abdominal cavity.
The finding of an enlarged Virchow’s node is referred to as Troisier’s sign – and indicates of the presence of cancer in the abdomen, specifically gastric cancer, that has spread through the lymph vessels.
Waldeyer’s Ring
Waldeyer’s tonsillar ring refers to the collection of lymphatic tissue surrounding the superior pharynx. This lymphatic tissue responds to pathogens that may be ingested or inhaled. The tonsils that make up the ring are as follows:
- Lingual tonsil – located on the posterior base of the tongue to form the antero-inferior part of the ring.
- Palatine tonsils – located on each side between the palatoglossal and palatopharyngeal arches. These are the common ‘tonsils’ that can be seen within the oral cavity. They form the lateral part of the ring.
- Tubal tonsils – these are located where each Eustachian tube opens into the nasopharynx and form the lateral part of the ring.
- Pharyngeal tonsil – also called the nasopharyngeal/adenoid tonsil, located in the roof of the nasopharynx, behind the uvulva and forms the postero-superior part of the ring.
Clinical Relevance: Inflamed Palatine Tonsils (Tonsillitis)
The palatine tonsils can become inflamed due to a viral or bacterial infection. In such a case, they appear red and enlarged, and are accompanied by enlarged jugulo-digastric lymph nodes.
Chronic infection of the palatine tonsils can be treated with their removal, a tonsillectomy. When performing a tonsillectomy, there may be bleeding primarily from the external palatine vein and secondarily from the tonsilar branch of the facial artery.
If an infection spreads to the peritonsillar tissue, it can cause abscess formation. This can cause deviation of the uvula, known as quinsy. A quinsy is a medical emergency, as it can potentially cause obstruction of the pharynx. It is treated with draining of the abscess and antibiotics.
Lymphatics of the Brain
It was thought that lymphatics were absent from the brain until in 2015, scientists located lymphatic vessels in the brains of mice and subsequently humans. Work is underway to determine and describe the lymphatic vessels involved.