The scrotum is a fibromuscular cutaneous sac, located between the penis and anus. It is dual-chambered, forming an expansion of the perineum.
Embryologically, the scrotum is derived from the paired genital swellings. During development, the genital swellings fuse in the midline – in the adult this fusion is marked by the scrotal raphe. The scrotum is biologically homologous to the labia majora.
In this article, we shall look at the anatomy of the scrotum – its contents, blood supply and innervation.
Contents
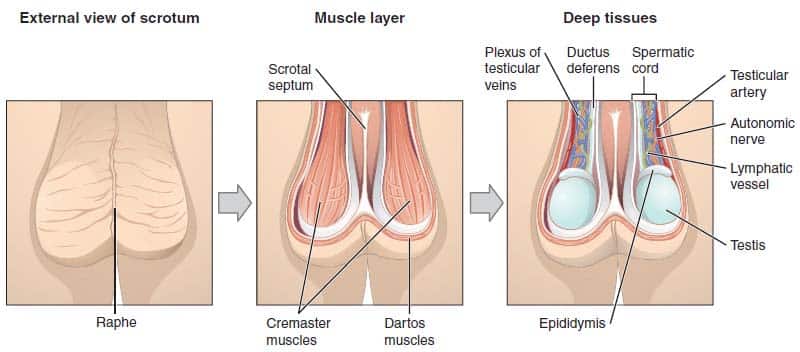
The scrotum contains three major (paired) structures:
- Testis – the site of sperm production.
- Epididymis – situated at the head of each testicle. It functions as a storage reservoir for sperm.
- Spermatic cord – a collection of muscle fibres, vessels, nerves and ducts that run to and from the testes.
There are also muscle fibres located within the scrotum. The dartos muscle is a sheet of smooth muscle, situated immediately underneath the skin. It acts to help regulate the temperature of the scrotum, by wrinkling the skin – this decreases surface area, reducing heat loss.
Neurovascular Supply
The scrotum receives neurovascular supply from the nearby vessels and nerves. This is in contrast to the testes – which carry their vessels, nerves and lymph drainage from the abdomen during their development.
Vessels
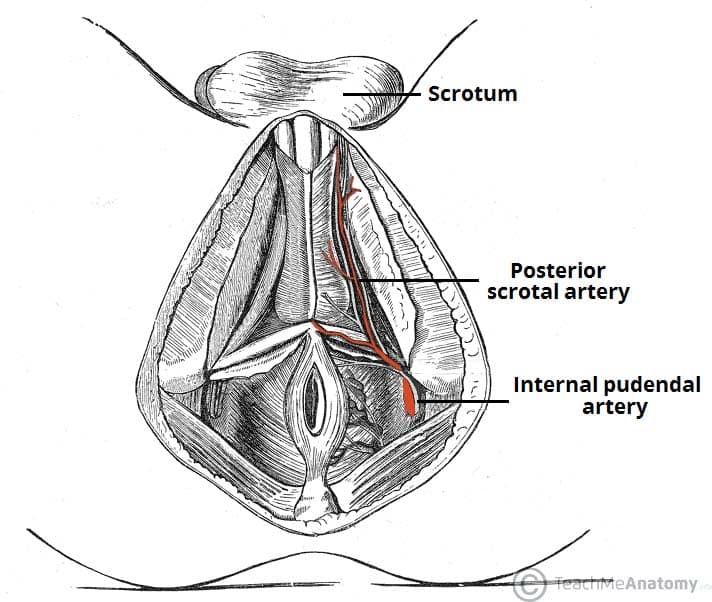
The scrotum receives arterial supply from the anterior and posterior scrotal arteries. The anterior scrotal artery arises from the external pudendal artery, while the posterior is derived from the internal pudendal artery.
The scrotal veins follow the major arteries, draining into the external pudendal veins.
Nerves
Cutaneous innervation to the scrotum is supplied via several nerves, according to the topography:
- Anterior and anterolateral aspect – Anterior scrotal nerves derived from the genital branch of genitofemoral nerve and ilioinguinal nerve
- Posterior aspect – Posterior scrotal nerves derived from the perineal branches of the pudendal nerve and posterior femoral cutaneous nerve.
Lymphatics
The lymphatic fluid from the scrotum drains to the nearby superficial inguinal nodes.
Clinical Relevance: Haematoma of the Scrotum
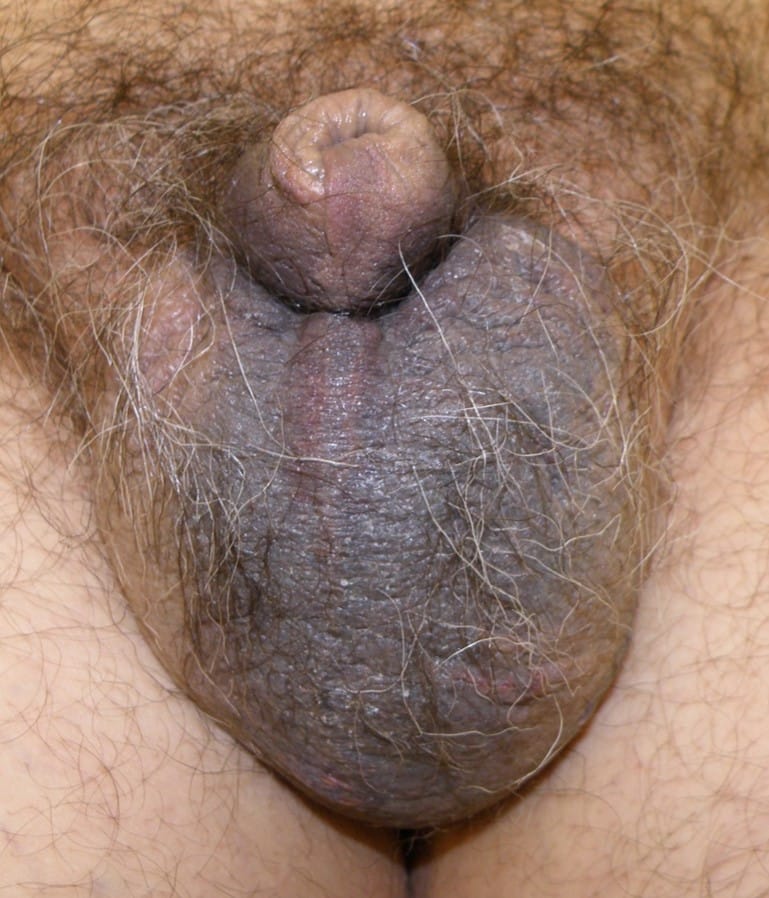
A haematoma may develop in the scrotum as a result of scrotal surgery or trauma in the genital region (Figure 3).
This results in swelling (oedema) and discolouration of the scrotal skin. Occasionally the origin of bleeding may not arise from the scrotal contents (i.e. spermatic cord and testis) but from the basal part of the penile urethra (the bulbar urethra) as in “straddle injuries” – direct perineal trauma like when falling onto a bicycle crossbar.