The uterus is a secondary sex organ. Secondary sex organs are components of the reproductive tract that mature during puberty under the influence of sex hormones produced from primary sex organs (the ovaries in females and the testes in males).
They are responsible for the maintenance and transportation of gametes.
In this article, we shall look at the composition and clinical significance of the uterus. Its vasculature, lymphatic supply and innervation will be covered.
Anatomical Structure
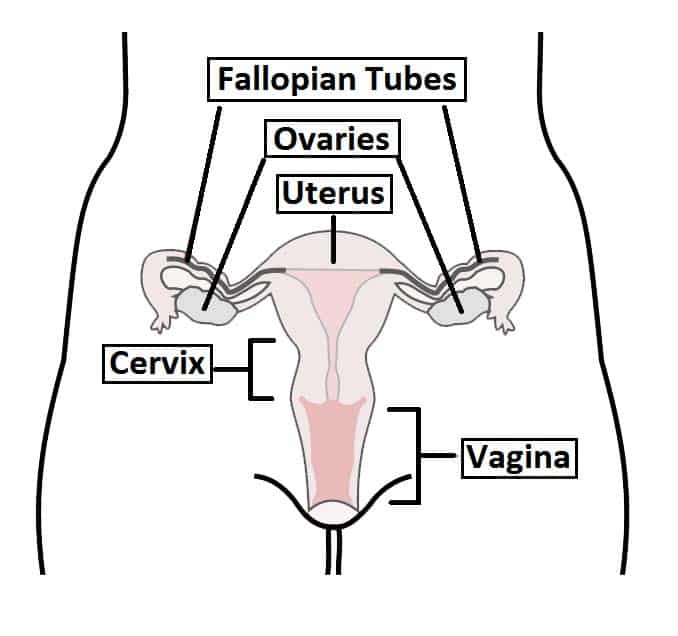
The uterus is a thick-walled muscular organ capable of expansion to accommodate a growing fetus. It is connected distally to the vagina, and laterally to the uterine tubes.
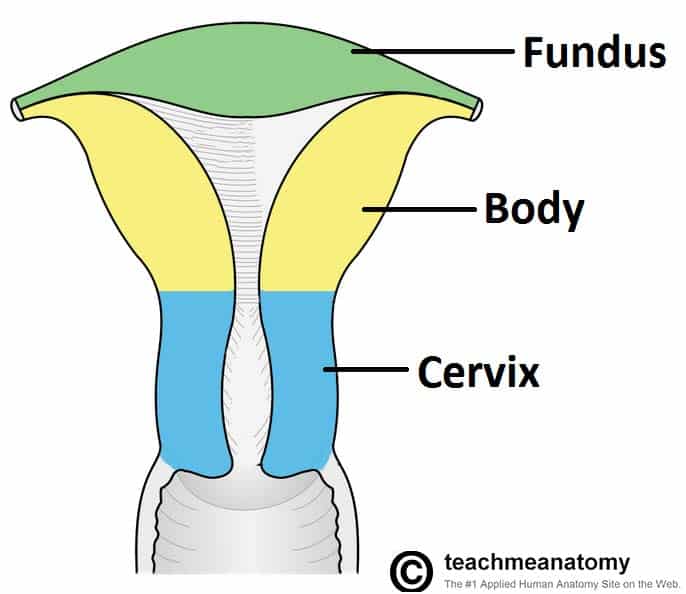
The uterus has three parts;
- Fundus – top of the uterus, above the entry point of the uterine tubes.
- Body – usual site for implantation of the blastocyst.
- Cervix – lower part of uterus linking it with the vagina. This part is structurally and functionally different to the rest of the uterus. See here for more information about the cervix.
Anatomical Position
The exact anatomical location of the uterus varies with the degree of distension of the bladder. In the normal adult uterus, it can be described as anteverted with respect to the vagina, and anteflexed with respect to the cervix:
- Anteverted: Rotated forward, towards the anterior surface of the body.
- Anteflexed: Flexed, towards the anterior surface of the body.
Thus, the uterus normally lies immediately posterosuperior to the bladder, and anterior to the rectum.
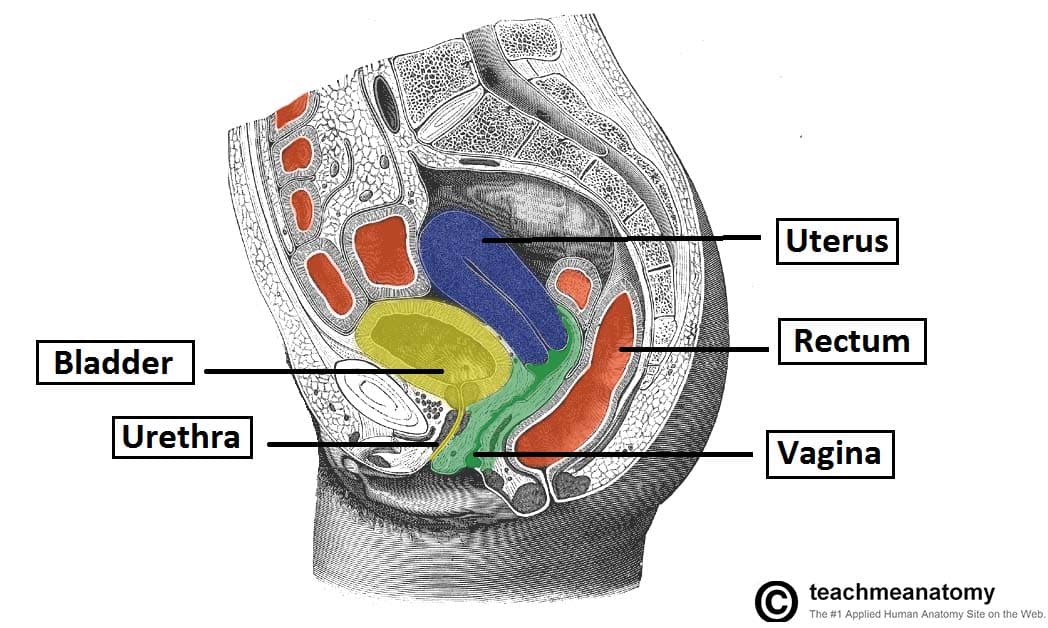
Fig 3 – Sagittal section of the female pelvis, showing the anatomical relations of the vagina.
Clinical Relevance: Abnormal Positioning of the Uterus
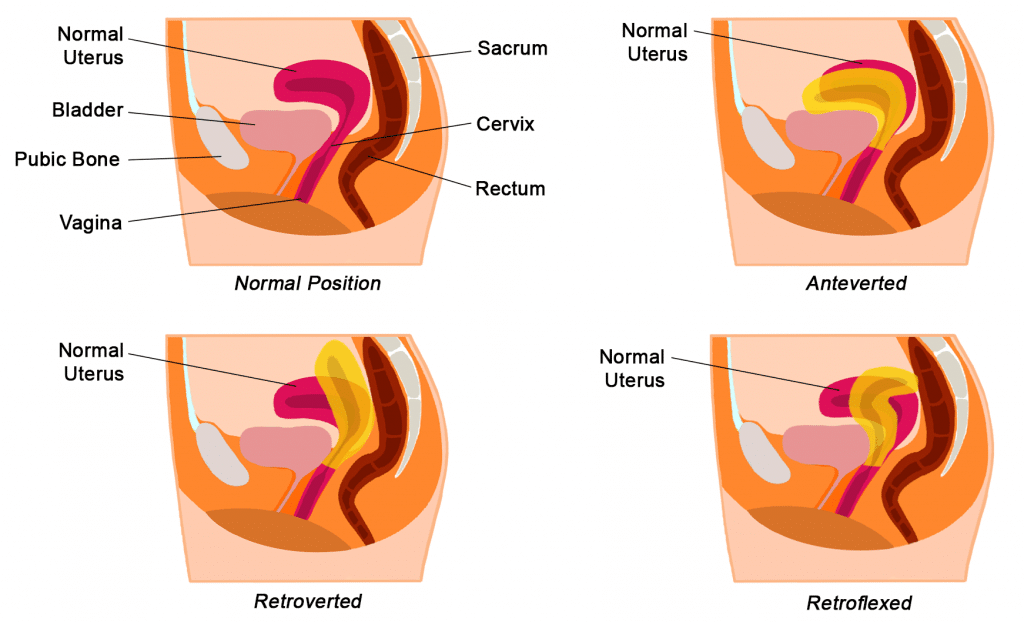
In some individuals, the uterus may not lie in an anteflexed and anteverted position. The three most common dispositions are:
- Excessively anteflexed
- Anteflexed and retroverted
- Retroflexed and retroverted
These abnormal arrangements do not inherently cause any medical problems. However, the retroverted uterus is positioned directly above the vagina. Thus in instances of increased abdominal pressure, the uterus is more likely to prolapse into the vagina.
Uterine prolapse is particularly prevalent in those with a history of pelvic floor damage.
Histological Structure
The fundus and body of the uterus are composed of three tissue layers;
- Peritoneum – a double layered membrane, continuous with the abdominal peritoneum. Also known as the perimetrium.
- Myometrium – thick smooth muscle layer. Cells of this layer undergo hypertrophy and hyperplasia during pregnancy in preparation to expel the fetus at birth.
- Endometrium – inner mucous membrane lining the uterus. It can be further subdivided into 2 parts:
- Deep stratum basalis: Changes little throughout the menstrual cycle and is not shed at menstruation.
- Superficial stratum functionalis: Proliferates in response to oestrogens, and becomes secretory in response to progesterone. It is shed during menstruation and regenerates from cells in the stratum basalis layer.
Ligaments
The tone of the pelvic floor provides the primary support for the uterus. Some ligaments provide further support, securing the uterus in place.
They are:
- Broad Ligament: This is a double layer of peritoneum attaching the sides of the uterus to the pelvis. It acts as a mesentery for the uterus and contributes to maintaining it in position.
- Round Ligament: A remnant of the gubernaculum extending from the uterine horns to the labia majora via the inguinal canal. It functions to maintain the anteverted position of the uterus.
- Ovarian Ligament: Joins the ovaries to the uterus.
- Cardinal Ligament: Located at the base of the broad ligament, the cardinal ligament extends from the cervix to the lateral pelvic walls. It contains the uterine artery and vein in addition to providing support to the uterus.
- Uterosacral Ligament: Extends from the cervix to the sacrum. It provides support to the uterus.
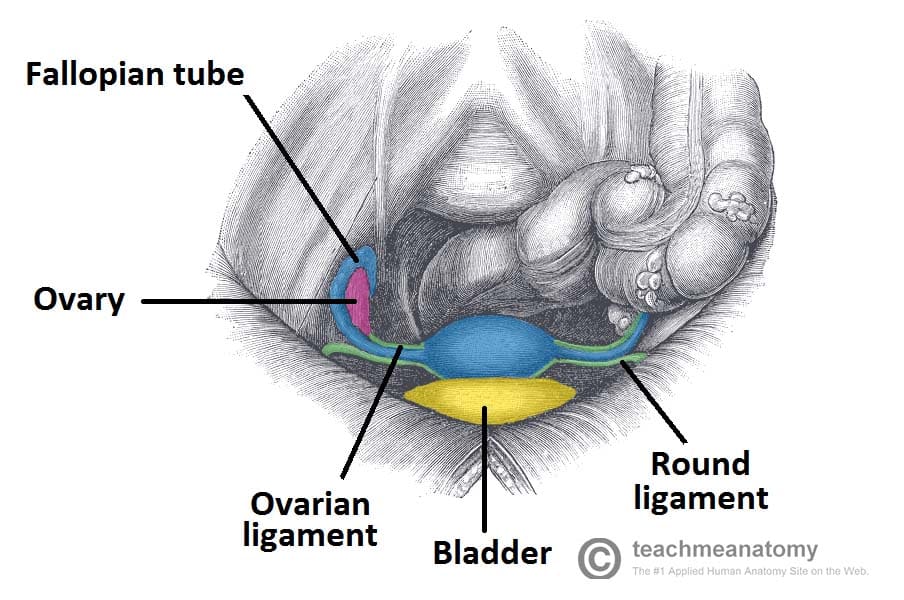
Fig 5 – Overview of the uterus and fallopian tubes, and associated ligaments
Vascular Supply and Lymphatics
The blood supply to the uterus is via the uterine artery. Venous drainage is via a plexus in the broad ligament that drains into the uterine veins.
Lymphatic drainage of the uterus is via the iliac, sacral, aortic and inguinal lymph nodes.
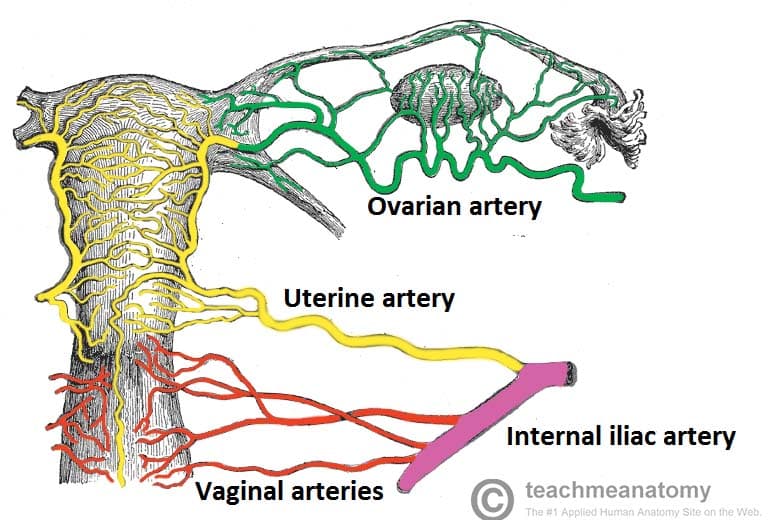
Fig 6 – Posterior view of the arterial supply to the female reproductive tract.
Clinical Correlation: Hysterectomy
A hysterectomy is the surgical removal of the uterus, usually as a result of cervical or uterine cancer.
When performing a hysterectomy, a good knowledge of regional anatomy is needed to prevent accidentally damaging other structures in the pelvic region.
The uterine artery crosses the ureters approximately 1 cm laterally to the internal os. Care must be taken not to damage the ureters during clamping of the uterine arteries during a hysterectomy. The relationship between the two can be remembered using the phrase ‘water under the bridge’. Water refers to the ureter (urine), and the uterine artery is the bridge.
Innervation
Sympathetic nerve fibres of the uterus arise from the uterovaginal plexus. This largely comprises the anterior and intermediate parts of the inferior hypogastric plexus.
Parasympathetic fibres of the uterus are derived from the pelvic splanchnic nerves (S2-S4).
The cervix is largely innervated by the inferior nerve fibres of the uterovaginal plexus.
The afferent fibres mostly ascend through the inferior hypogastric plexus to enter the spinal cord via T10-T12 and L1 nerve fibres.
Clinical Correlation: Disorders of the Endometrium
Endometriosis is the presence of ectopic endometrial tissue at sites outside the uterus, most commonly the ovaries and the ligaments of the uterus. Ectopic tissue is still responsive to oestrogenic stimuli therefore cyclic proliferation and bleeding occur, often forming a cyst. The condition is associated with dysmenorrhoea and/or infertility.
Fibroids are benign tumours of the myometrium which affect 20% of menopausal women. They are oestrogen dependent, enlarging during pregnancy and with use of the contraceptive pill but regressing after the menopause. Most fibroids are asymptomatic, but if large enough the uterine mass can cause symptoms including menorrhagia, pelvic pain and infertility.
Endometrial carcinoma is the most common malignancy of the female genital tract, most often found during, or after, the menopause, and characterised by abnormal uterine bleeding.