The rectum is the most distal segment of the large intestine, and has an important role as a temporary store of faeces.
It is continuous proximally with the sigmoid colon, and terminates into the anal canal.
In this article we will discuss the anatomy of the rectum – its structure, anatomical relationships, and clinical relevance.
Anatomical Structure
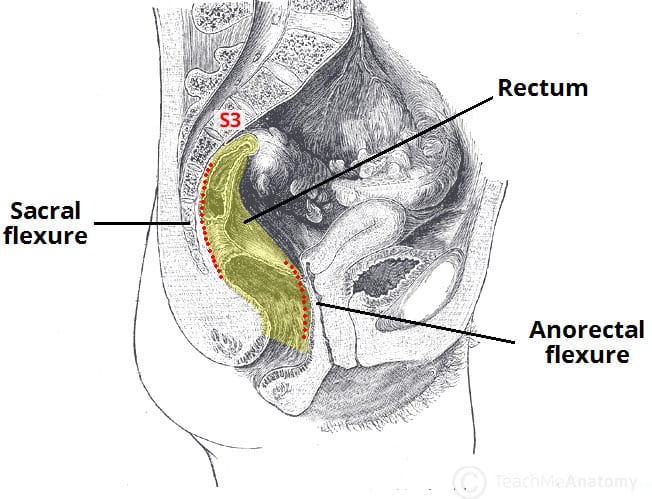
The rectum begins at the level of the S3 (as a continuation of the sigmoid colon). It is macroscopically distinct from the colon, with an absence of taenia coli, haustra, and omental appendices.
The course of the rectum is marked by two major flexures:
- Sacral flexure – anteroposterior curve with concavity anteriorly (follows the curve of the sacrum and coccyx).
- Anorectal flexure – anteroposterior curve with convexity anteriorly. This flexure is formed by the tone of the puborectalis muscle, and contributes significantly to faecal continence.
There are additionally three lateral flexures (superior, intermediate and inferior), which are formed by transverse folds of the internal rectum wall.
The final segment of the rectum, the ampulla, relaxes to accumulate and temporarily store faeces until defecation occurs. It is continuous with the anal canal; which passes through the pelvic floor to end as the anus.
Peritoneal Coverings
In the superior third of the rectum, the anterior surface and lateral sides are covered by peritoneum. The middle third only has an anterior peritoneal covering, and the lower 1/3 has no peritoneum associated with it.
In males, the reflection of peritoneum from the rectum to the posterior bladder wall forms the rectovesical pouch. In females, the peritoneum reflects to the posterior vagina and cervix, forming the rectouterine pouch (pouch of Douglas). See more about the peritoneal cavity here.
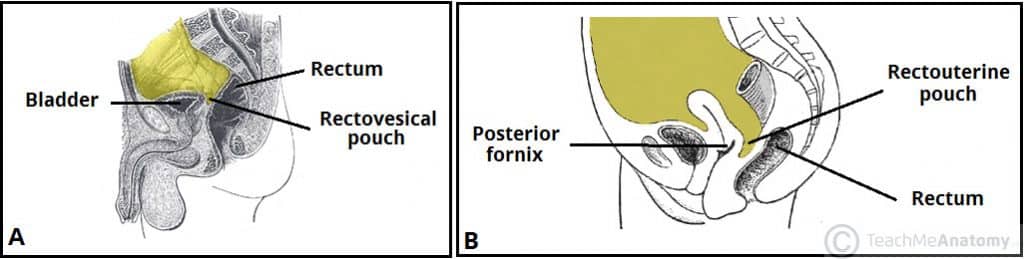
Fig 2 – The peritoneal reflections of the rectum in males (A) and females (B).
Anatomical Relations
The rectum is located within the pelvic cavity, and is the most posterior of the pelvic viscera. Its anatomical relations are different in men and women:
Anterior |
Posterior |
|
| Male | Female | Sacrum and coccyx |
| Rectovesical pouch | Rectouterine pouch | |
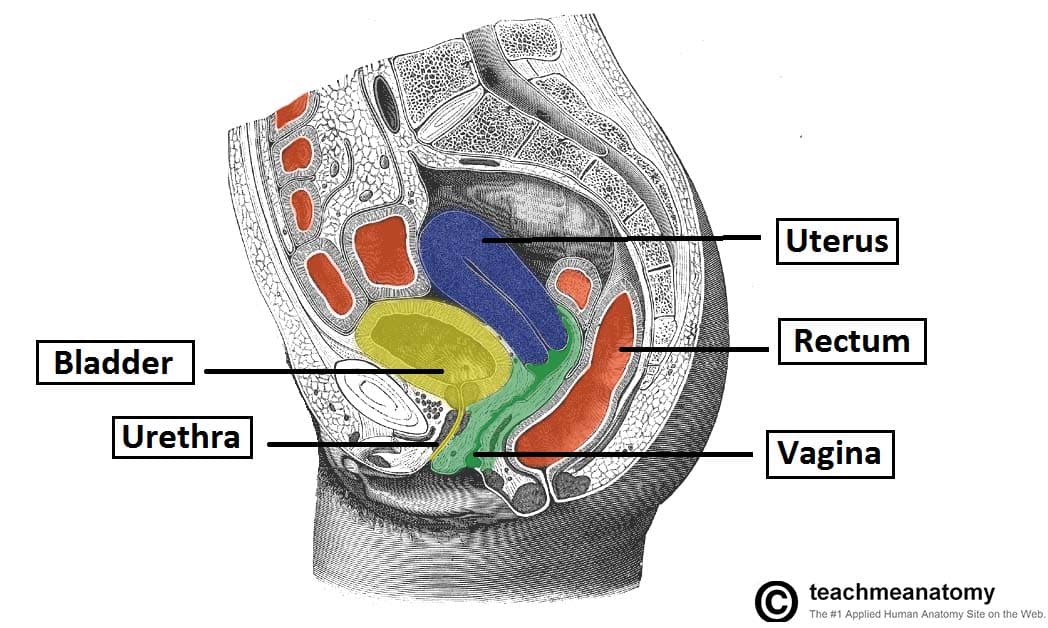
Fig 3 – Sagittal section of the female pelvis, showing the anatomical position of the rectum.
Neurovascular Supply
The rectum receives arterial supply through three main arteries:
- Superior rectal artery – terminal continuation of the inferior mesenteric artery.
- Middle rectal artery – branch of the internal iliac artery.
- Inferior rectal artery – branch of the internal pudendal artery.
Venous drainage is via the corresponding superior, middle and inferior rectal veins. The superior rectal vein empties into the portal venous system, whilst the middle and inferior rectal veins empty into the systemic venous system. Anastomoses between the portal and systemic veins are located in the wall of anal canal, making this a site of portocaval anastomosis.
Note: the rectum is also closely anatomically associated with the rectal venous plexus; however this structure is more functionally related to the anal canal.
Innervation
The rectum receives sensory and autonomic innervation.
Sympathetic nervous supply to the rectum is from the lumbar splanchnic nerves and superior and inferior hypogastric plexuses. Parasympathetic supply is from S2-4 via the pelvic splanchnic nerves and inferior hypogastric plexuses. Visceral afferent (sensory) fibres follow the parasympathetic supply.
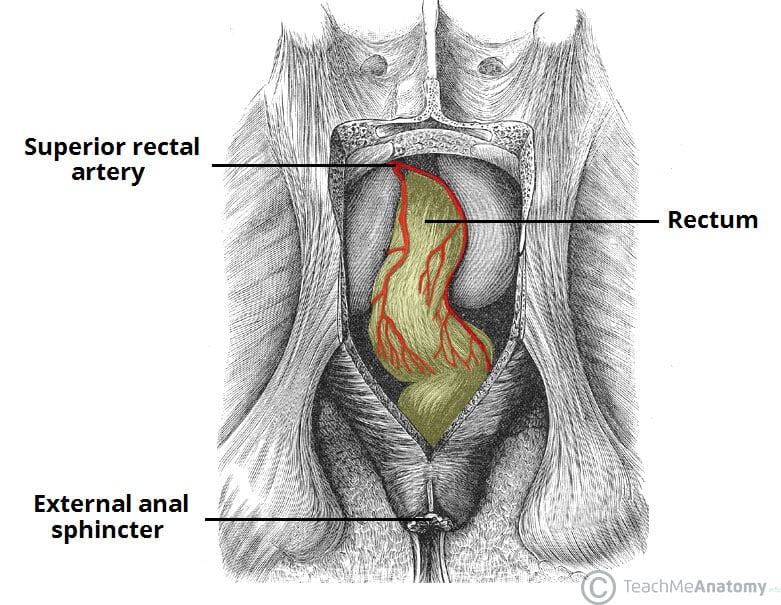
Fig 4 – The superior rectal artery, supplying the upper aspect of the rectum.
Lymphatic Drainage
Lymphatic drainage of the rectum is via the pararectal lymph nodes, which drain into the inferior mesenteric nodes.
Additionally, the lymph from the lower aspect of the rectum drains directly into the internal iliac lymph nodes.
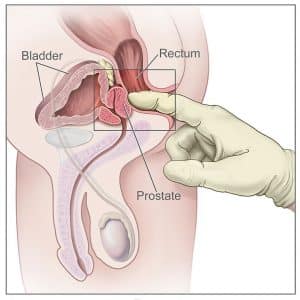
Clinical Relevance – Digital Rectal Examination
The anterior wall of the rectum has a number of close anatomical structures. These can therefore be palpated digitally via the rectum. Most significant are the prostate and seminal vesicles in males, and cervix in females. Bony structures, such as the sacrum and coccyx, may also be palpated in both sexes.
For a guide on performing a digital rectal examination, visit our sister site TeachMeSurgery.